Up-to-date radiological knowledge
Whether you work as a general practitioner or medical specialist, whether you are a resident or an intern, or if you simply want to expand your knowledge in your medical and paramedical profession: the Radiology.expert platform will provide all the practical radiological expertise that you need for proper interpretation & diagnosis of imaging studies. The training modules, developed by a radiologist, will bring your radiological knowledge up to the required standard.
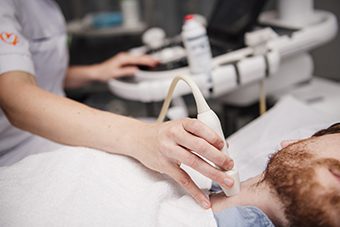
Learn the general basics of the radiology discipline, with a special focus on the various examination techniques.
View all modules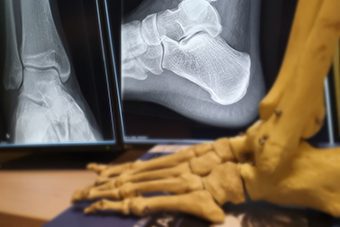
Search for the part of the body that you are interested in and learn all you need to know about the corresponding radiological examination.
View all modules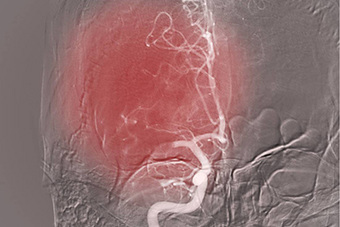
Interventional radiology is a rapidly evolving medical specialty: learn the core principles, techniques, and clinical applications.
View all modulesWhy you should choose Radiology.expert
Radiology.expert offers a helping hand, to assist you in the correct interpretation and diagnosis of imaging studies. Using specific examples, we will explain how radiological images & scans should be assessed and you will learn the ins and outs of the radiology discipline.
- Access to over 20 high-quality modules
- Reliable up-to-date expertise from the radiologist
- Specific situations and experiences
- Can be applied quickly & correctly in practice
user experiences of radiology.expert
Expertise for all
Learn about the most important items that are relevant to you in a short period of time. From basic knowledge about the various basic techniques to radiological knowledge per professional field or per part of the body. Select the radiological knowledge and module that suits you best. You can complete the module once you have purchased it. You can also subscribe so that you will have access to all modules.
- Choose a module or put together your own package of modules
- Personal login account
- 1 year unlimited access
- Save interesting modules
- Unlimited access to all modules
- Personal login account
- 1 year unlimited access
- Save interesting modules
request
- Access to all modules
- Multiple login accounts
- Best choice for educational institutions










 Fracture general principles
Fracture general principles
 Ultrasound Technique
Ultrasound Technique
 MRI Lumbar Spine
MRI Lumbar Spine
 Chest X-ray
Chest X-ray
 CT abdomen general
CT abdomen general
 X-Hip
X-Hip
 Abdominal ultrasound
Abdominal ultrasound
 Abdominal X-ray
Abdominal X-ray
 Bone tumours
Bone tumours
 CT sinus
CT sinus



